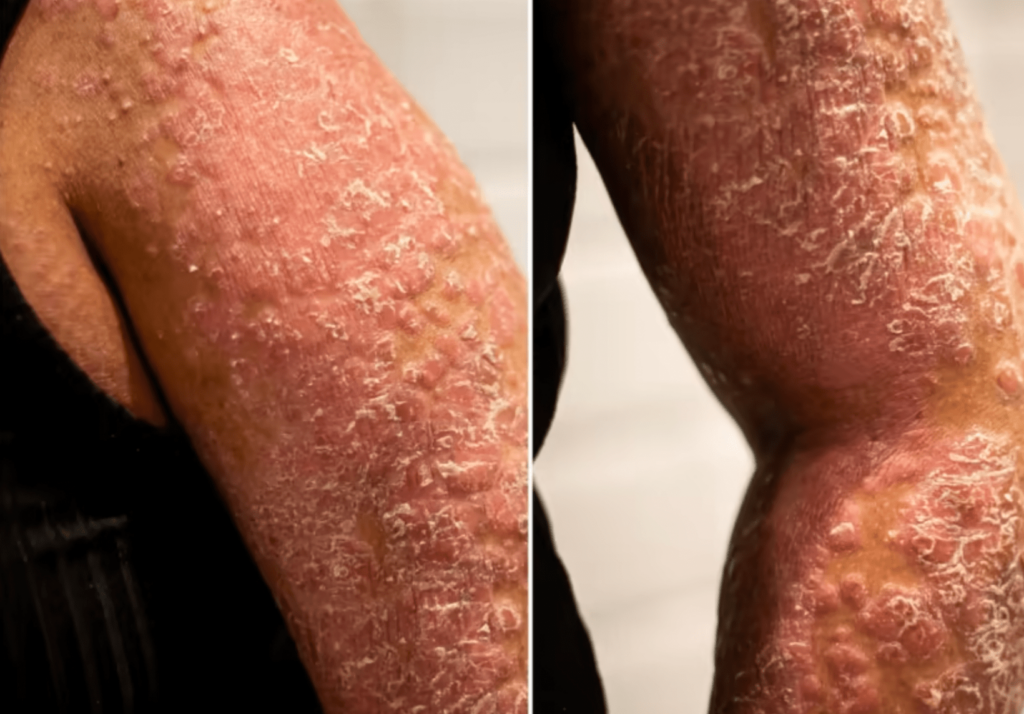
Close-up views of the arm of Ms Emmylou Casanova, who suffers from generalised pustular psoriasis. This was after a flare-up of the disease, which is not contagious.
When angry-looking red patches of skin first appeared on Ms Mei Yetti Roslan’s scalp and skin, her neighbours told her that she was “cursed”.
She was 16 then. At 49 years old now, Ms Mei said that the painful skin lesions she has been suffering from since young “still feel like a curse”.
“I believed it at the time because I was the only one (among friends, neighbours and relatives) who has it,” she said.
The Singapore permanent resident, who is from Indonesia, has an autoinflammatory skin disease called generalised pustular psoriasis (GPP).
The incurable and potentially life-threatening condition is an acute and severe form of psoriasis, a chronic autoimmune skin disorder. It is not contagious.
When the disease flares up — usually suddenly and without warning — red, painful and blister-like sores bulging with pus take over large areas of the skin.
They itch, burn and hurt so bad that the slightest movement would feel excruciatingly painful.
For Ms Mei, who now works as an assistant teacher, the flare-ups can get so severe that she would need to be hospitalised. In 2019, she was admitted to the intensive care unit here due to complications from the disease.
Recalling the particularly severe episode in 2019, she said that her entire body and skin felt like they were burning.
“I would cry every night. I couldn’t sleep, I couldn’t move my body (because of the pain),” she told TODAY.
Earlier this month, Ms Mei and other patient advocates from the region raised awareness of the disease at a media roundtable discussion hosted by biopharmaceutical company Boehringer Ingelheim, at the World Congress of Dermatology Singapore 2023.
The event also showcased an art collection by Dutch designer Bart Hess that was inspired by the experiences of people living with GPP.
Dr Colin Theng, president of the Psoriasis Association of Singapore, said that once a person develops the disease, it is for life. There is no cure, although treatments can help control the symptoms.
Around 40,000 people are living with psoriasis in Singapore. Less than 1 per cent have this severe acute form.
Dr Theng is also a councillor with the International Psoriasis Council.
NO ORDINARY PAIN
The exact cause of GPP is not known but it is believed to have a genetic component. Mutations in the IL-36RN gene have been found to be associated with the disease, Dr Theng said.
“Activation of this (IL-36) pathway leads to inflammation, and this can cause systemic symptoms seen in GPP,” he said.
Stress, certain medications, hormonal changes during pregnancy, or sudden withdrawal from steroids, for example, may also trigger GPP.
Patient advocate Emmylou Casanova, 46, who has been living with GPP for almost two decades, said that the condition has affected all aspects of her life. Severe episodes have left her bedridden, affecting her emotionally and financially. “Living with GPP is a psychological, social and emotional torture. Patients not only endure the excruciating pain from a flare-up, but we also tend to withdraw from society to avoid being discriminated against”
An International Federation of Psoriasis Associations’ ambassador from the Philippines, Ms Casanova highlighted the need to raise awareness of GPP and provide avenues for patients to “voice their pain”.
The federation is a global non-profit organisation made up of national and regional psoriasis patient associations around the world.
“When we have a flare-up, we can’t do anything by ourselves — not even going to the toilet,” Ms Casanova said, having experienced a recent flare-up herself.
To show TODAY the highly visible skin symptoms that can go on for weeks or months after a flare-up, Ms Casanova removed her jacket, revealing widespread painful lesions on her arms.
“Living with GPP is a psychological, social and emotional torture. Patients not only endure the excruciating pain from a flare-up, but we also tend to withdraw from society to avoid being discriminated against,” she said.
Ms Mei said that the pus-filled lesions that occur are sometimes accompanied by a “bad smell”, much “like rotten fish”.
GPP pustules contain pus, a white or yellow fluid filled with white blood cells.
Dr Theng explained that there may be an odour when a secondary bacterial infection sets in, which is why patients should not scratch the infected area and practise good hygiene to manage the condition.
“Getting proper medical treatment to control the disease will be the most important measure because once the condition is under control, the skin odour will be cleared, too,” he said.
SEPSIS, ORGAN FAILURE
Dr Theng said that the under-recognised skin disease is often mistaken for other conditions such as a skin infection or allergy, or the more common plaque psoriasis, which is also an autoimmune disease that causes dry, itchy and raised patches (plaques) on the skin that are covered with whitish dead skins cells.
Last year, a study published in the American Journal of Clinical Dermatology found that more than half (59 per cent) of the people who have GPP were misdiagnosed at first.
This may lead to delays in treatment, which can have life-threatening implications.
Plaque psoriasis is the most common type of psoriasis, but it is a distinctly different disease from GPP.
With GPP, symptoms are more than just skin-deep. It is not uncommon for patients to require emergency hospital care whenever they get a flare-up.
Alongside skin symptoms, Dr Theng said that patients also experience systemic features such as fever, headaches, extreme tiredness, joint pain and muscle weakness — features not typically seen in the more common form of psoriasis.
“Patients can become septic and have low blood pressure, and this can be life-threatening. GPP can also cause organ damage, for example, to the liver, lungs, heart and kidney,” he added.
Dr Theng has observed that many patients turn to alternative medicine, such as Traditional Chinese Medicine, or try different types of home remedies advised by well-meaning family or friends.
“Unfortunately, most of these treatments do not work, and some treatments can irritate and aggravate the skin condition. Furthermore, this can lead to a delay in seeking proper medical treatment, which can have devastating consequences for the patient,” he said.
NEEDING LIFELONG TREATMENT
While some patients may require treatment only when the disease flares, others may need to be on treatment for life.
Dr Theng said that the goal of treatment is to make symptoms less severe so that patients can heal faster, resume their daily activities, and avoid complications that may require hospitalisation.
Traditional treatments for GPP include oral medications (such as methotrexate, acitretin and cyclosporine) that can control the disease.
Not all patients respond optimally to the treatments either.
The latest treatment for psoriasis involves the use of biologic treatments (such as TNF-alpha inhibitors, IL17a inhibitor and IL23 inhibitors) that are approved for plaque psoriasis, but have been used in GPP with good success, Dr Theng added.
Biological therapy works by targeting the parts of the immune system that are triggering inflammation that causes diseases such as autoimmune disorders.
Dr Theng said: “There are now new biologic treatments for psoriasis that have been specifically developed for pustular psoriasis. They target the IL36 receptor, which is a key player in the pathway that drives GPP, and have been found to be very effective and safe.
“So, there may be more opportunities to help control flares in the future.”
For Ms Mei, treatment has helped control her symptoms, allowing her to continue with her daily activities and work. However, her search for an effective treatment has come at a cost to her fertility.
In 2016, while seeking treatment in Indonesia, she was prescribed a medication called methotrexate that reduces the overactivity of the immune system.
Dr Theng said that the medication, which is now among the treatment options for GPP, should not be given to women who are planning to get pregnant because it can cause miscarriages and affect the normal development of the foetus.
Ms Mei said that her menstrual periods stopped after taking the medication for six months, affecting her ability to conceive after her marriage to a Singaporean warehouse assistant in 2018.
“I still hope to have a child. Every Mothers’ Day, I’ll always feel sad.”
Her husband, Mr Roslan Mohamed, 53, said: “Having a child is important to us, but what to do? Maybe there will be a miracle.”




